A bat bite is often so small you might not even see it — it can look like a tiny pinprick, a thin scratch, or two small red dots close together, and that's exactly what makes it so dangerous.
Bat bites are one of the most frequently missed animal injuries in emergency medicine. The teeth of most bat species are needle-thin, meaning they can puncture skin without causing the bleeding or pain you'd normally associate with an animal bite.
Many people who are bitten don't realize it happened at all. In the United States, bats are the leading source of human rabies deaths, with the Centers for Disease Control and Prevention (CDC) reporting that most fatal rabies cases in recent decades were linked to bat exposure. Even a bite that looks like nothing — barely a scratch — needs immediate medical attention. This is not a wait-and-see situation.
I reviewed dozens of clinical case reports and emergency medicine guidelines to put this together. What I found was that the danger isn't in how the bite looks but in the fact that it's easy to dismiss entirely.
What Does a Bat Bite Actually Look Like?
The Classic Appearance
Most bat bites are genuinely tiny. We're talking about marks that can be as small as 1 to 2 millimeters across. In clinical settings, a bat bite typically presents as one or two small puncture wounds, sometimes surrounded by a faint ring of redness.
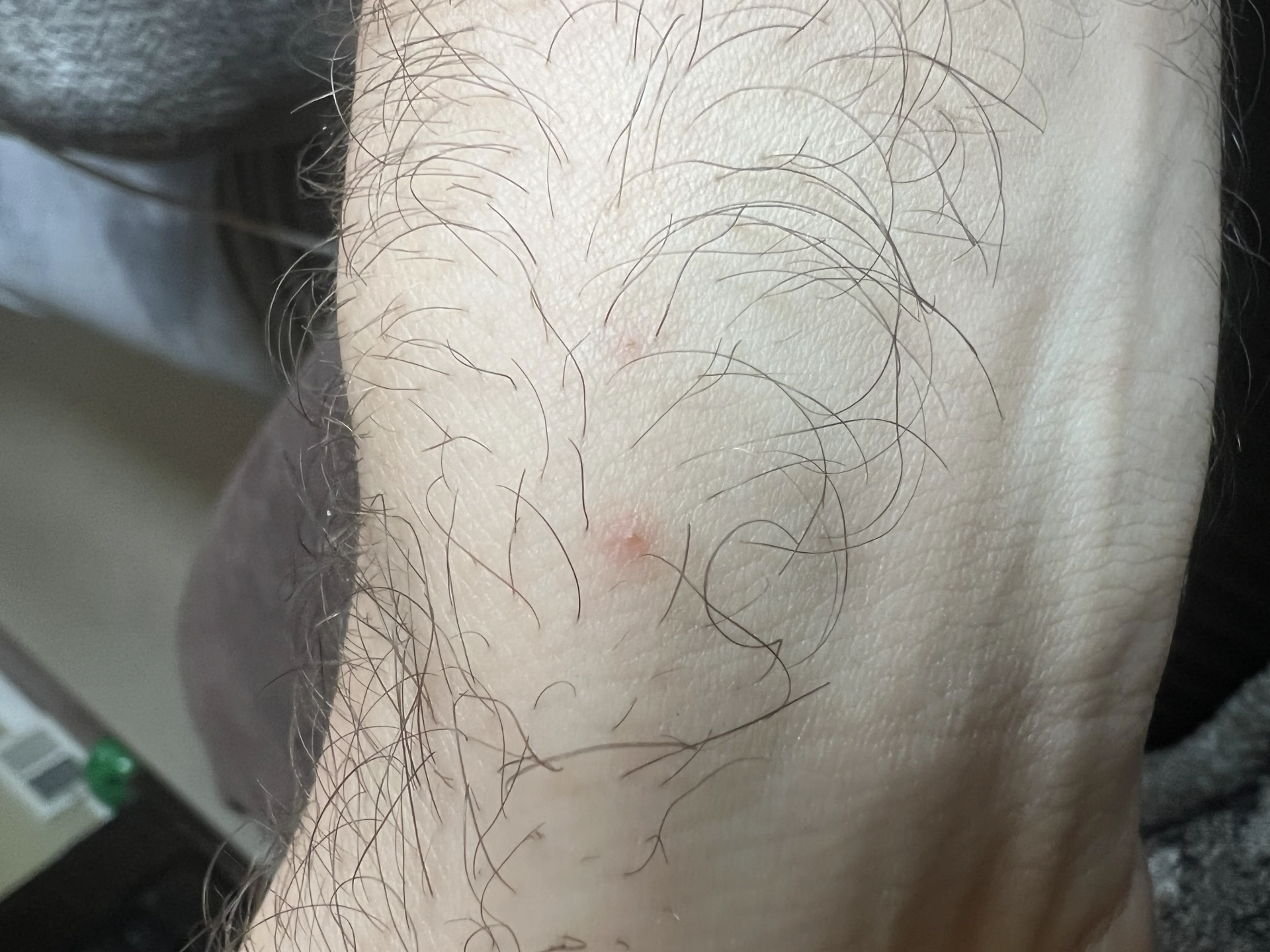
You might see a thin scratch-like line if the bat dragged its teeth sideways, or two pinprick dots side by side if the teeth entered cleanly.
The wound rarely bleeds heavily. Because bat teeth are so fine, they slide through the outer layers of skin with minimal tissue damage. This is very different from a dog bite or a cat scratch, which are usually obvious and painful.
When the Bite Is Invisible
Here's the part that surprises most people: in a significant portion of bat-exposure cases, no visible wound is found at all. The CDC specifically acknowledges scenarios where a person woke up to find a bat in their room, or a bat was found near a sleeping child or pet, and no mark could be located on the skin.
In these cases, medical authorities in the U.S. and UK still recommend treating the situation as a potential exposure and seeking post-exposure prophylaxis (PEP).
I looked at emergency department case studies, and a recurring theme was patients saying "I didn't feel anything, so I figured I was fine." That assumption has cost lives.
Color and Texture Changes Around the Bite
In the hours after a bat bite, the skin around the wound may show:
- Slight redness or pinkness in a small halo around the entry point
- Minor swelling, rarely more than a few millimeters
- A bruise-like discoloration in very rare cases where the bat bit harder
The area typically doesn't look infected in the early stages. Any sign of pus, expanding redness, warmth, or red streaking appearing later may indicate a secondary bacterial infection and requires separate antibiotic treatment.
How to Tell a Bat Bite Apart From Other Injuries
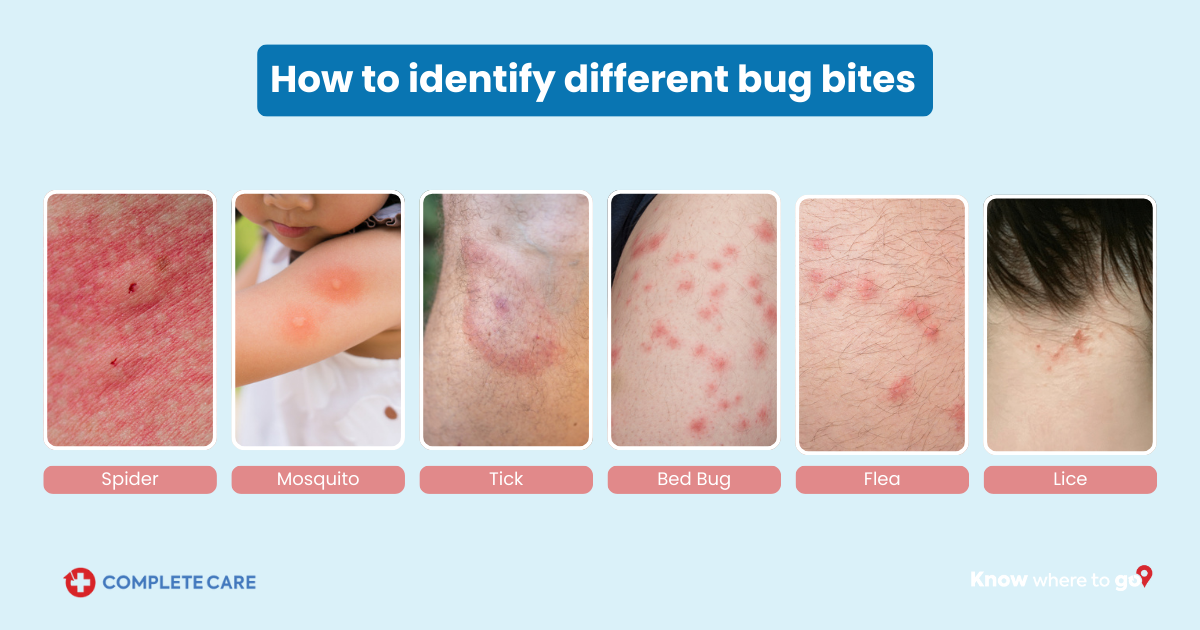
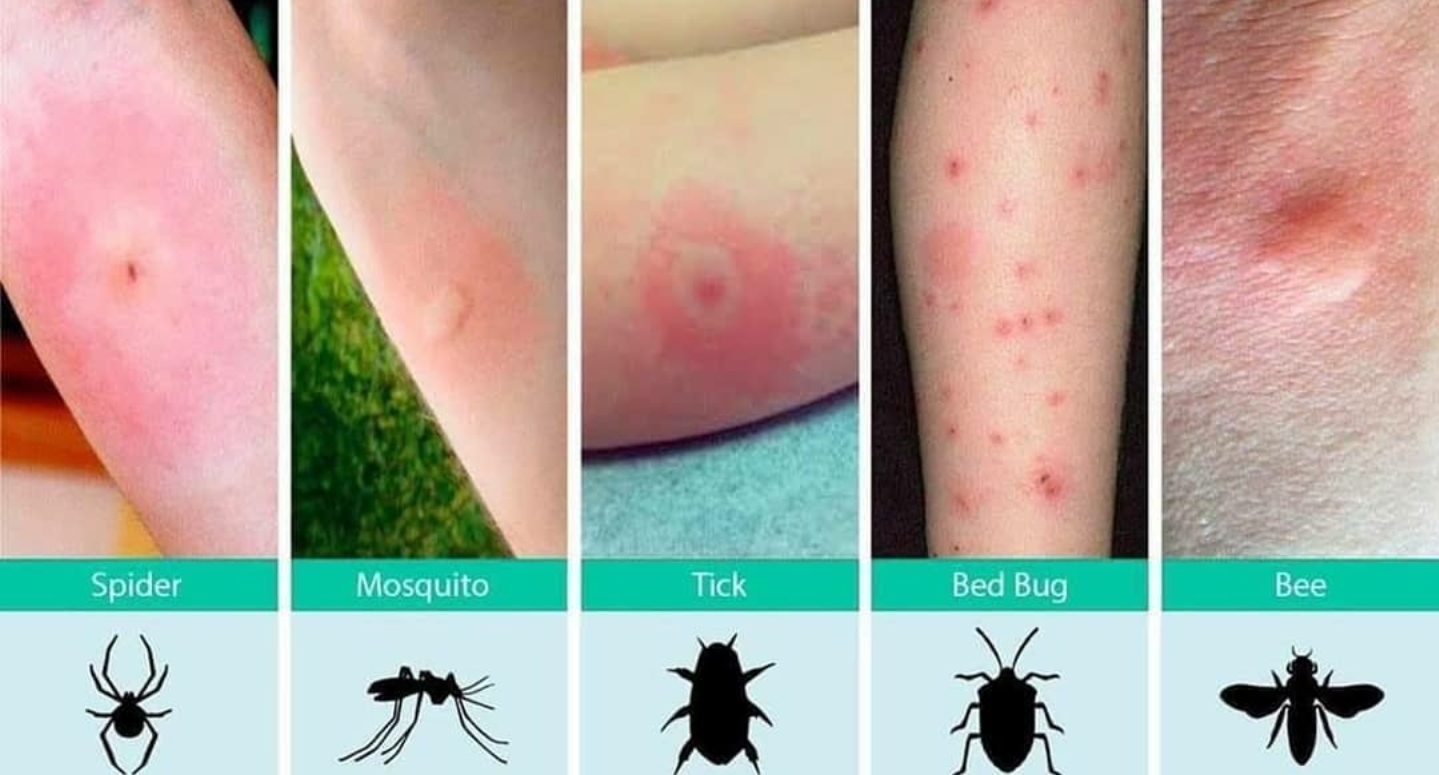
Bat Bite vs. Insect Bite
Insect bites from mosquitoes or fleas tend to raise a visible welt with a central red dot and noticeable itching. A bat bite looks flatter and doesn't typically itch. There are usually two puncture marks very close together with a bat, reflecting the spacing of the upper and lower canine teeth, whereas most insect bites are single points.
Bat Bite vs. Cat Scratch
Cat scratches are longer, often parallel, and more superficial. They tend to bleed a bit and sting. A bat bite is rounder and deeper relative to its size. If you woke up and found a thin scratch you can't explain, and there was a bat nearby, treat it as a bat bite.
Bat Bite vs. Thorn or Splinter
This is one of the most common mix-ups. People often dismiss a bat bite as something they caught on a branch or fence. The key difference is location: bites tend to appear on the hands, arms, feet, or face, and they come in pairs, not singles.
A quick real-world example: A colleague of mine in rural Wales told me about waking up one summer morning with what looked like a tiny scratch on her index finger. She assumed it was from gardening the night before. It wasn't until she mentioned finding a pipistrelle bat stunned on her windowsill that her GP immediately referred her for PEP. The mark was less than 3mm long and had no redness at all. She described it as something she would have ignored on any other day.
Bat Bite Symptoms: What Happens to Your Body
Immediate Symptoms (First 24 Hours)
In most cases, a bat bite causes very little immediate reaction. You might notice:
- A faint stinging or tingling at the site
- Mild warmth around the wound
- No bleeding, or very minimal bleeding that stops within minutes
These subdued symptoms are part of what makes bat bites medically tricky. The human immune system doesn't raise an obvious alarm in the way it does with larger wounds.
Signs of Rabies Infection (If Untreated)
If a bite is not treated and the bat was rabid, the rabies virus travels along nerve pathways toward the brain. The incubation period can range from a few weeks to over a year, though most cases present symptoms within 1 to 3 months.
Early neurological symptoms include:
- Fever and headache (often mistaken for flu)
- Pain, burning, or itching specifically at the old bite site
- Anxiety, confusion, and agitation
- Hydrophobia (fear of water, caused by painful throat spasms)
- Aerophobia (fear of air drafts)
Once these symptoms appear, rabies is almost always fatal. This is why the "it looks like nothing" argument carries so much weight in medical circles. The window for effective treatment is before symptoms start.
Secondary Bacterial Infection Symptoms
Bats carry a range of bacteria in their mouths, including Pasteurella multocida and Capnocytophaga species. A secondary infection may cause:
- Increasing pain and swelling over 12 to 48 hours
- Warmth and redness spreading outward from the wound
- Pus or discharge from the puncture site
- Fever and chills
These bacterial infections are treatable with antibiotics, but they still require medical care.
What to Do Right After a Bat Bite
Step 1: Clean the Wound Immediately

Wash the bite site with soap and water for at least 15 minutes. This one step alone has been shown in studies to significantly reduce the risk of rabies transmission. Do not scrub hard enough to cause more tissue damage, but be thorough.
Step 2: Do Not Wait to Seek Care
Go to an emergency department or urgent care clinic the same day. Bring as much information as you can: where the bat was, whether it was acting strangely, whether you could catch it for testing.
Step 3: Ask About Post-Exposure Prophylaxis (PEP)
PEP for rabies consists of a series of vaccine doses and, for people who have never been vaccinated before, a one-time dose of rabies immunoglobulin (RIG). When started promptly after exposure, PEP is nearly 100% effective at preventing rabies. Once symptoms develop, there is no effective treatment.
Step 4: Report the Bat
Contact your local animal control or public health authority. If the bat can be safely captured without further exposure, it may be tested for rabies, which can confirm or rule out the need for full PEP.
Common Misconceptions and Risks
"If I Don't Feel Pain, I Wasn't Bitten"
This is the most dangerous myth. Bat teeth are so fine and sharp that many bites are truly painless. People bitten while sleeping may never feel anything. The absence of pain is not evidence of the absence of a bite.
"Bats Only Attack If Provoked"
A bat that bites a person, especially during daytime or in an unusual location, may be sick. Healthy bats almost never make contact with humans. A bat that approaches people, cannot fly properly, or is found on the ground should be treated as potentially rabid.
"I Was Wearing Gloves, So I'm Fine"
Standard gardening or work gloves are not adequate protection against bat bites. Bat teeth can penetrate thin fabric. Only thick leather gloves designed for animal handling provide reliable protection.
"Rabies Is Rare, So It's Not Worth Worrying About"
Bat-associated rabies strains are responsible for the majority of human rabies deaths in North America. While the total case count is low, the fatality rate once symptomatic is effectively 100%. The rarity of the disease does not reduce the need for prompt action after any exposure.
Related Concepts and Entities
Understanding bat bites connects to several broader topics in medicine, public health, and wildlife management. The key medical concepts include post-exposure prophylaxis (PEP), zoonotic disease transmission, and wound infection management.
The primary public health entities involved are the CDC (Centers for Disease Control and Prevention) in the U.S., Public Health England (now the UK Health Security Agency, or UKHSA), and the World Health Organization (WHO), which classifies rabies as a neglected tropical disease and maintains global guidance on its prevention.
Bat species most commonly involved in human exposure in the UK include the common pipistrelle (Pipistrellus pipistrellus), while in the U.S., species like the big brown bat (Eptesicus fuscus) and little brown bat (Myotis lucifugus) are frequent culprits. In the UK, the European Bat Lyssavirus (EBLV), a rabies-related virus, is the primary concern rather than classical rabies.
Wildlife management and conservation context is important too. Bats are protected species in the UK under the Wildlife and Countryside Act 1981 and in many U.S. states. This means you cannot kill or disturb them, which sometimes creates conflict when people find bats roosting near living spaces. Knowing how to safely contact a bat handler or report a bat without harming it is part of responsible exposure management.
Frequently Asked Questions
Can a bat bite be completely invisible?
Yes. The CDC explicitly states that some bat bites leave no visible mark. This is especially true when the bite occurs during sleep, when the person may not have moved or reacted. If you wake up and find a bat in your room, or if a bat was found near a child or pet, treat it as a potential exposure even without a visible wound.
How long after a bat bite do rabies symptoms appear?
The rabies incubation period is highly variable. Most human cases develop symptoms within 1 to 3 months, but documented cases have shown symptoms emerging anywhere from 10 days to over a year after exposure. The length of incubation may relate to the location of the bite (bites closer to the brain tend to progress faster) and the amount of virus introduced.
Should I try to catch the bat that bit me?
If it can be done safely without further exposure, yes. A bat that can be tested and confirmed negative for rabies can eliminate the need for full PEP treatment. Use thick leather gloves or a container to trap it, do not handle it with bare hands, and contact your local health authority or animal control for guidance on getting it tested.
Is a bat bite dangerous in the UK even without classical rabies?
Yes. In the UK, bats can carry the European Bat Lyssavirus (EBLV), which is closely related to the rabies virus and causes a rabies-like illness. PEP is recommended in the UK for any confirmed or likely bat bite, and the UKHSA maintains specific guidance for bat-related exposures. There have been bat-associated lyssavirus deaths in the UK, making this a real concern even without classical rabies being present.
Do I need a tetanus shot after a bat bite?
Possibly. If your tetanus vaccination is not up to date, a booster may be recommended after any animal bite, including a bat bite. Your doctor will assess this as part of the initial evaluation. Tetanus is separate from the rabies PEP protocol but is an important part of wound care.
What if I touched a bat with my bare hands but was not visibly bitten?
This should still be reported to a healthcare provider. Bat bites can occur through casual contact without the person realizing it. Scratches from bat claws are also considered a potential rabies exposure route, as are mucous membrane contacts (eyes, nose, mouth) with bat saliva. Your doctor will assess the exposure and decide whether PEP is appropriate.
Final Thoughts
A bat bite is genuinely one of those injuries where the smallest-looking wound carries the most serious consequences. The mark may be barely visible, or invisible entirely, and the immediate symptoms may be almost nothing, but the potential outcome if left untreated is as serious as medicine gets. Whether you spotted a tiny double pinprick on your hand, woke up to find a bat in your room, or just aren't sure what happened, the right call is always the same: clean the area, head to a doctor that day, and ask specifically about PEP. Getting treatment you might not need is a small inconvenience; skipping treatment you do need is a decision that cannot be undone.
References
- Centers for Disease Control and Prevention (CDC). "Rabies: Bats." https://www.cdc.gov/rabies/exposure/animals/bats.html
- World Health Organization (WHO). "Rabies Fact Sheet." https://www.who.int/news-room/fact-sheets/detail/rabies
- UK Health Security Agency (UKHSA). "Rabies: Guidance, Data and Analysis." https://www.gov.uk/guidance/rabies-guidance-data-and-analysis
- Rupprecht CE, et al. "Rabies and Rabies Virus." Infectious Disease Clinics of North America. 2021. https://www.id.theclinics.com
- Manning SE, et al. "Human Rabies Prevention — United States, 2008." MMWR Recommendations and Reports. CDC. https://www.cdc.gov/mmwr/preview/mmwrhtml/rr5703a1.htm
- Wildlife and Countryside Act 1981 (UK). legislation.gov.uk. https://www.legislation.gov.uk/ukpga/1981/69/contents
- Public Health England. "Rabies: Epidemiology in the UK." 2019. https://www.gov.uk/government/publications/rabies-epidemiology-in-the-uk
- Hampson K, et al. "Estimating the Global Burden of Endemic Canine Rabies." PLOS Neglected Tropical Diseases. 2015. https://doi.org/10.1371/journal.pntd.0003709
